Almanac Health is a clinical AI platform that brings specialist-grade knowledge to clinicians at the point of care — providing evidence-based clinical decision support across medical specialties, free from pharmaceutical advertising, and governed by institutional controls. The platform integrates with existing EHR systems and is clinically validated through peer-reviewed research. Almanac Health was founded by Cyril Zakka, MD, author of one of NEJM AI’s most-cited papers on retrieval-augmented generation for clinical medicine.
Sector: Healthtech + Services
Alder
Alder offers expert, hands-on support for families navigating the complexities of aging. Alder is a team of experienced social workers and nurses helping families navigate the complexities of aging with compassion, clarity, and hands-on support.
Nikhil Marathe
Nikhil is a Principal at F-Prime, where he spearheads the firm’s efforts in healthcare growth equity. His primary focus is to partner with rapidly growing, capital efficient businesses in healthcare software and services.
Prior to joining F-Prime, Nikhil worked at Juxtapose, a creation-oriented investment firm focused on healthcare and technology, where he spent 2 years incubating a new business venture in the pharmaceutical services ecosystem. Prior to Juxtapose, Nikhil spent 13 years at Silversmith Capital Partners and TA Associates, where he closed 12 growth-stage investments across healthcare and enterprise software. He began his career as a technology investment banker at Evercore.
Nikhil has a BS in Economics from The Wharton School at the University of Pennsylvania, with concentrations in Finance and Management.
Behind the Breakthrough: Q&A with Kai Eberhardt, CEO and Co-founder of Oviva
Kai Eberhardt transformed a personal cancer diagnosis in his twenties into a lifelong commitment to improving patient empowerment and healthcare accessibility.
Diagnosed with cancer in his early twenties, Kai Eberhardt quickly learned how disheartening it can feel to navigate the healthcare system without information or agency. That experience became a transformational force, first pushing him toward deeper medical knowledge, then through a PhD in medical physics, and ultimately into the business of healthcare.
He co-founded Oviva in 2014 with engineer Manuel Baumann to confront one of the most widespread, but underserved, health challenges in society: chronic weight-related conditions (such as obesity and type 2 diabetes). Despite the abundance of clinical evidence showing that behavior change and lifestyle interventions can be highly effective, few systems were designed to deliver them at scale, and even fewer offered sustained, patient-centric care accessible to everyday lives.
Eberhardt and his team saw an opportunity to reimagine care delivery, starting with something simple: a secure, compliant chat app connecting patients and their care teams. Over time, that communication layer evolved into Oviva’s full-stack digital care platform, now used by more than one million patients across the UK and Europe.
On the heels of Oviva’s expansion into cardio-metabolic conditions, and after nearly a decade of building credibility and capability in systems like the National Health Service (NHS), Eberhardt shares what it takes to turn frustration into innovation, how the company is scaling with purpose, and why technology is only one part of the solution.
What gap in the healthcare system were you aiming to address in founding Oviva?
The idea for Oviva emerged from a common challenge in obesity treatment—most patients don’t continue treatment after one or two visits. It just isn’t practical for patients to regularly attend sessions in-person despite a demand for care.
What stood out was that these same patients were always on their phones, and unlike other areas of care, weight management doesn’t require physical exams, lab work, or imaging. It largely includes education, coaching, and real-time support. So, we asked: what if we digitized the same care that we provided in-person and delivered it on their phones, anytime, anywhere? That would make it dramatically more accessible, and likely more effective, too.
Can you talk more about how this model helps address affordability and equity?
People managing chronic conditions often juggle jobs, childcare, daily stress – and weight-related health is important, but not always urgent. That makes it easy to de-prioritize care, especially when it requires a visit to a doctor’s office on a random Wednesday afternoon.
Making care available on your phone, on your own schedule, changes everything. For example, look at the NHS Diabetes Prevention Programme – about 20% of people completed the in-person model, but closer to 70% completed Oviva’s digital version. That’s a massive difference.
Virtual care also opens the door to serving culturally and linguistically diverse communities. With digital delivery, you can tailor the content, language, and nutrition guidance for many different patients. Curating care is almost impossible to do well in a one-size-fits-all, in-person group setting.
You integrate clinical, nutritional, and psychological care. What makes that approach so essential?
Obesity is multifactorial – you just can’t treat it through one lens. Some people need help with nutrition education, some have complex psychological patterns or trauma, and now we also have powerful medications that should be managed by doctors. No one discipline can cover it all.
Not every patient needs every service, but having a full stack available is essential to delivering effective care. We learned this from the best in-person programs –where coordination across teams made all the difference, though it was resource-intensive and hard to sustain. By operating digitally, we can bring those same multidisciplinary perspectives together without the limits of geography or scheduling.
What makes Oviva truly different from other players in your space?
We’re with our patients every day. That’s the biggest difference. Face-to-face models might give you 30 minutes with a clinician once a month. We’re a daily companion – logging meals, giving feedback, coaching, and support throughout the day. That consistency leads to better outcomes.
We’ve published more than 90 papers showing that we outperform in-person care, and because we’re digital, we can do it at lower cost and with broader reach. We’re essentially industrializing something that used to be artisanal – making personalized, behavior-change therapy highly scalable.
Regarding Oviva’s role within the NHS – what does it take to build innovation and credibility in a system as rigorous and complex as that one?
Evidence, first and foremost. I’ve always believed in backing up what we do with strong data, while publishing results publicly to build trust and demonstrate transparency.
After that, it’s about communication – having the skills and patience to speak to very different stakeholders across the NHS. And finally, it’s about partnership. We don’t try to replace services; we instead think about how we can add value to the system through better access and efficiency. This mindset helps us prove we’re here for the long haul.
You have talked about being driven by your own personal experiences in the healthcare space. Can you share how that energy helped shape your journey as a founder?
I’ve always been a pretty intense and action-oriented person. Frustration, for me, serves as a powerful motivator because it offers clarity and urgency. I don’t sit still when I see something broken. I’m not afraid to make decisions or move fast. I think that drive helped me do something many would consider irrational – starting a health tech company from the ground up in a pretty complex space.
Obesity is a field that often carries judgment or stigma. How do you lead with compassion and evidence in that environment?
Honestly, that’s one of the most fulfilling parts of what we do. Many of our patients haven’t received good care before – they’ve been judged or dismissed by the system. When we help them see real progress, it’s incredibly rewarding.
It’s not just for the patient’s benefit either. We’ve shown, with data, that our program reduces patient sick days by about a third within six months. That translates to added productivity in the workplace, tax revenue, and long-term cost savings – things that help the entire system. So, when people ask if this population is “worth investing in,” our results make the answer abundantly clear.
What advice would you give to other founders trying to build something in or alongside a public health system?
You need grit. It takes a long time to get through validation, adoption, and scaling inside a system like the NHS. The process can be very frustrating, especially when you know your solution could help people immediately, but adoption takes time.
Some delays are for good reasons, like needing strong evidence. Other delays are due to competing interests or systemic inertia. You must keep showing up and pushing forward. The reward is that once you’re in, and your model works, it’s incredibly sticky and impactful.
What excites you the most about what’s coming next?
We’re about to launch our hypertension solution, pending final regulatory approvals. It’s been in the works for two years and is a huge opportunity to build something that serves both patients and doctors more effectively – especially in how we manage data, daily insights, and ongoing support between visits.
The role of AI in all of this is just getting started. Our AI-first care model has the potential to transform patient support, making delivery more efficient and effective. We can provide even better continuity of care between doctor visits and better inform doctors for those visits. Since the ChatGPT moment, we’ve been embedding more AI features into our product, making care more scalable and improving outcomes. AI technology and Oviva are evolving rapidly – and I can’t wait to see how far we can go.
Olivia Carlson
Olivia Carlson is a Senior Associate at F-Prime, focusing on investments in healthcare technology and services companies. Prior to joining F-Prime, she was an investor at M33 Growth, where she assessed investment opportunities and supported their portfolio of growth-stage healthcare companies. Olivia also worked in strategy consulting for EY-Parthenon’s healthcare team. She started her career as a certified nursing assistant, working for a home health and hospice company throughout college.
Olivia holds a B.A. from Williams College, where she majored in Pre-Medical Studies and Psychology.
F-Prime’s Summer Internship and Fellowship Program: Meet Our 2025 Interns and Fellows
A big thank you to our interns and fellows for their valuable contributions this summer!
This summer, F-Prime was excited to welcome a talented group of interns and fellows to our Cambridge and London offices. They played key roles in competitive landscape analysis, sourcing, founder calls, and more. Read on to discover what it’s like to be part of our internship and fellowship programs.

“This experience has deepened that interest, especially seeing how these tools might fit into real business contexts like VC. Listening to discussions where those kinds of possibilities are explored has also been hugely motivating. ”

“The work is creative. I expected rigorous diligence, but I didn’t anticipate how much of the job involves pattern recognition, storytelling, and forming contrarian but grounded views on where a field is heading. You’re constantly toggling between scientific depth and high-level strategic vision.”

“I am most surprised by how fast-paced and rapidly evolving the job is. The team has many new calls every day, while also having to study new technologies, keep up with the news, and manage the portfolio companies. I am learning a great deal about how to manage all these aspects of being a venture capitalist.”

“I have come to further appreciate how the venture framework is about asking the right questions rather than having all the answers. The best investors seem to pair scientific curiosity with disciplined judgment, which has given me a deeper appreciation for how to approach underwriting risk.”

“One thing that stood out is how hands-on and multidimensional the team is at every level. I expected sharp and high-level strategic thinking from partners, but it was refreshing to see just how engaged they are in the details; in every meeting, building models, debating sourcing strategies, refining TAMs.“

“I was most surprised by the rapid pace of innovation and how quickly the team collaborates to evaluate and act on exciting new opportunities. I also learned how important building relationships are in the VC world. it’s not only about finding good investments but also about fostering long-term relationships with founders and industry leaders.”

“I learned about F-Prime through a family friend. I decided to join as an intern because F-Prime gets to work with amazing biotech startups and help them grow as a business. Additionally, the culture at F-Prime is extremely friendly and everyone at the firm wants to help you be the best version of yourself.”
Applications for our 2026 program are not open yet, but if you are interested in learning more, please send an email to careers@fprimecapital.com.
From Shortages to Scale: Specialty Care in the AI Era
AmplifyMD’s $20M Series B fuels platform for scalable virtual specialty care.
We spend $1 of every $5 in the U.S. economy on healthcare. That’s exorbitant compared to most developed countries, where people live longer than we do at half the cost. Perverse incentives continue to drive unsustainable cost growth, with employer plans expected to grow by more than 9% in 2026. Our current model reduces employee take-home pay and saddles future generations with added debts to pay for today’s inefficient, fragmented system.
We need startups to clean up this unmanageable mess. To disrupt the current system, entrepreneurs must challenge health oligopolies (e.g., insurance carriers, PBMs, health systems) and chip away at the economic rent extracted by overpaid intermediaries (e.g., brokers, provider contractors, revenue cycle vendors). They also must build new platforms to enable efficient care delivery, powered by AI.
Provider shortages abound because the medical profession has long operated under an oligopoly and guild mentality, limiting the number of new physicians trained each year. Fortunately, technology now allows vastly more efficient distribution of provider time and talent, which could ultimately reverse the expected scarcity. The pandemic proved that care can be delivered effectively in virtual settings, despite primitive tools. As data has also become more portable, we may finally see the end of an era where provider systems hoard data to keep patients in high-cost settings and preserve unfair pricing power. Advances in software now allow “systems of engagement” to interface seamlessly with legacy “systems of record.” This opens the door to disrupting EHR monoliths and creating “new moats,” with AI poised to inject powerful new capabilities into outdated infrastructure.
These shifts create fertile ground for new platforms built for a digital-first, data-rich era, representing a new digital care architecture. AmplifyMD is one such platform – and today we’re thrilled to announce its $20M Series B financing. As an AmplifyMD director, I’ve seen firsthand how its EHR-integrated, AI-enabled virtual care platform helps health systems extend scarce physician capacity and drive material operational efficiencies. AmplifyMD allows specialists to practice anywhere, virtually treating patients in acute care settings and beyond, via its state-of-the-art platform. What began as a solution to expand specialist access in underserved settings has become a systemwide coverage solution trusted by some of the nation’s largest health systems—enabling physicians to extend their expertise without geographic limits.
The age of AI will further transform AmplifyMD’s product into an essential aspect of efficient and effective care delivery. The advent of superintelligent AI in medicine presents a golden opportunity for “creative destruction” to take root, but its potential requires modern platforms like AmplifyMD, which shift workflows from the in-person setting to always-on digital infrastructure. AI can enhance productivity and quality through clinical decision support today, and over time, may enable increasingly autonomous care delivery. This will give patients a greater ability to participate in decisions while receiving tailored treatment plans.
In the modern architecture of care delivery, AI agents will likely evolve to do the heavy lifting for all of us, freeing providers to focus on the highest leverage moments. With innovations like AmplifyMD’s platform, powered by this new financing, the industry can move toward greater access to high-quality care – an important step toward a system that respects our limits today while unlocking our innovative potential for tomorrow.
Axle Health
Axle Health is a healthcare technology company on a mission to revolutionize home-based care delivery through its comprehensive operations platform. Founded in 2020 by healthcare and technology veterans, including several former Uber executives who brought their logistics expertise to the healthcare industry, Axle Health’s AI-powered logistics platform enables healthcare organizations to efficiently deploy clinicians for in-home visits, improving patient outcomes while reducing operational costs. The company is headquartered in Los Angeles, California.
Gold-standard Eating Disorder Treatment Delivers Lasting Recovery for Patients and Families at Home
In 2019, Kristina Saffran and Dr. Erin Parks came to us with a slide deck and a passion for helping those struggling with eating disorders (EDs).
We were drawn to their story and mission as many of our team members had been touched by EDs – either suffering from one themselves or having a loved one who had struggled with an ED. Some are surprised to learn that EDs are the most expensive and one of the deadliest behavioral health conditions in the U.S., second only to opioid addiction. Nearly 30 million Americans across all races, genders, body sizes, and sexual orientations will have an eating disorder in their lifetime. Despite their prevalence, only 20% of those struggling receive treatment, and even less have access to evidence-based treatment. Our shared commitment to address this critical treatment gap, coupled with our strong belief in Kristina and Erin, led to our partnership with Equip.
We were delighted to lead the seed round that helped bring Kristina and Erin’s vision to life and to support them through the early fundamentals of company creation, including advising them through decisions about how to incorporate the company. Our team also had the pleasure of helping name the company – we proposed “Equip” during the naming process, believing that it reflected the ethos of the company. Equip – based on equipe, meaning “team” in French and the idea that the company has a strong focus on helping patients figure out how to equip themselves with skills to turn to instead of harmful behaviors. One of our team members, Brooke Hammer, even ultimately joined the company as a key member of the leadership team.
“F-Prime was one of our original champions who truly allowed Equip’s bold vision to become a reality. We, and the eating disorder field, are forever grateful for them.”
Kristina Saffran, CEO and Co-founder
Equip is positioned to transform eating disorder treatment with compelling evidence that their clinical approach works for lasting recovery. A remarkable 96% of Equip’s patients on a weight restoration program are gaining weight, 7 out of 10 are seeing reduction in their ED symptoms and 80% of parents have reported an increased confidence in their ability to address their child’s ED.
Eating disorder treatment is complex and cannot be one-size-fits-all. Equip’s medical and behavioral health platform is built to meet patients and families where they are through virtual family-based therapy (FBT). There are still significant challenges in the space but Equip is leading the way to deliver accessible, effective, fully virtual care.
The Four AI Agents of Your Health
With the advent of AI, we are only beginning to envision how dramatically it will change the management of our health.
Many people have already used Claude, Gemini or ChatGPT to evaluate symptoms or interpret lab results. As models, apps, and users evolve, the possibilities to alter how care is delivered, accessed, and financed seem limitless.
From Carbon to Silicon
To fully grasp how AI might change healthcare, we first need to understand how our current system — built around humans and analog methods — limits our potential. Our health system was constructed on the assumption that information is stored locally in proprietary archives (on paper or in locally controlled EHRs), and that knowledge is stored in the minds and hands of trained providers.
In 1999, The Institute of Medicine showed that more than 100,000 people were dying annually due to medical errors. Since then, clinicians and administrators have sought to resolve flaws in our system. With AI, we may be able to rethink care delivery to resolve these problems, freeing us from the bottlenecks of a limited human supply of trained clinicians. The architects of hospitals and insurance companies never imagined that silicon could transcend carbon, yet the early days of generative AI make it obvious that this technology will transform the way care is delivered. AI-related tools can play an important role in reducing patient harm, while making our system more affordable and accessible.
Overcoming the Limits of Imagination
With new technologies, there is often a failure of imagination; society has a collective inability to see how the world can be reshaped by breakthrough innovations. This can be because new technologies are immature and the infrastructure to scale them does not yet exist. It is also due to humanity needing time to understand how to take advantage of new things. As Chris Dixon has commented, when the film camera was invented, creators needed a long time to figure out you could do more than just film a staged play indoors. In healthcare, changes in the way physicians practice often require the retirement of one cohort of doctors and the rise of a new generation of providers, who are more comfortable with newer tools (as was seen with the adoption of less invasive, laparoscopic surgery).
Adaptation Requires Creative Destruction
Beyond the limits of imagination, administrators face practical barriers to change. How can one be sure it is safe, legal, or appropriate to use new AI technologies? If providers automate current processes, such as replacing in-person care with an AI-enabled app or digital therapeutic, how can they backfill lost revenue associated with redundant activities? Will the data AI depends on be available and exchangeable without sacrificing privacy and security?
Our healthcare system isn’t designed with accessible data as a core assumption. More than a pragmatic challenge, this is a business model issue: large health systems would prefer that you never leave their four walls (which they call “patient leakage”), because they operate as oligopolies, leveraging market power to get better rates from payers. And yet, our health journeys take us outside of those four walls, where our data is no longer available, integrated, or complete.
For the modern potential of AI to truly advantage everyone, there needs to be a new architecture for data that enables this future. Truly ubiquitous data will make services more readily available and of higher quality, while also enabling a marketplace of care solutions that are not held back by fear of data blocking. If data integration were simple, patients (and their primary care providers and navigators) could evaluate cost vs. quality and the forces of creative destruction would reshape services, lowering costs.
The Four AI Agents of Your Health
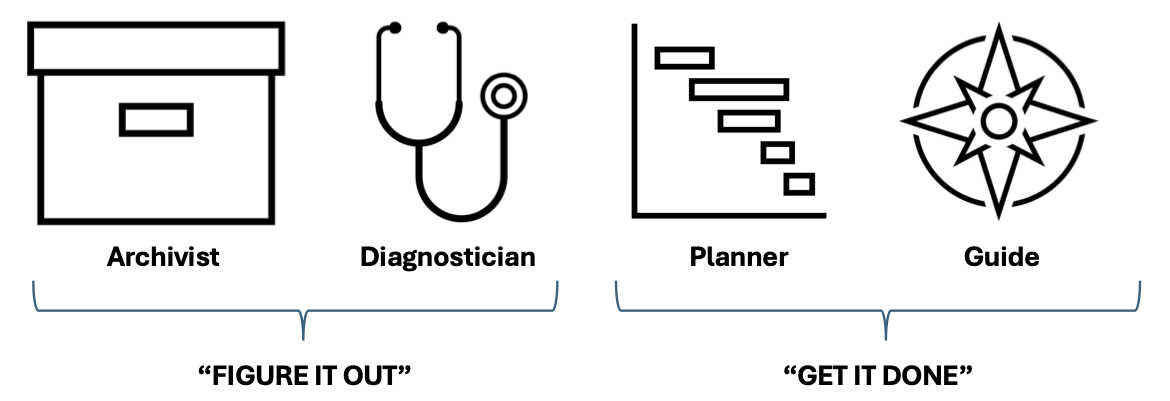
In an AI-enabled future powered by a new data architecture, four “agents” are likely to emerge, who will work together to improve our health – four different objective functions that will be part of each patient’s life in an efficient and effective health care future. This framework originates from a straightforward concept that one must analyze the state of events and then orchestrate actions based on that understanding. This was stated memorably by Jay Desai, who would tell his team to “figure it out” and “get it done.” Jay’s charge is a great way to organize the work of managing health: figure it out, and get it done.
In terms of “figuring it out,” two agents will be key.

Moving from the realm of “figuring it out” to “getting it done,” two other agents become important in your life.

Four Bots for the Win
One might note that the four bots could, in fact, be one larger AI system operating cohesively, and this is likely. The reason it’s helpful to separate these four agents initially is to emphasize that these are four different objective functions, which work together. The Archivist aims to ensure the record is always complete. Whenever new items enter the archive, this is a prompt for The Diagnostician to update the risk assessment, just as new medical knowledge continues to improve its foundation model. An updated risk assessment could then prompt The Planner to adjust the health plan for a given patient. In turn, a change in the plan will require The Guide to update the user accordingly. The sequence of tasks could go the other way as well. Perhaps The Guide is told by the user that a new bout of scalp pain is occurring, prompting it to alert the other three bots and make appropriate adjustments. Perhaps The Diagnostician calls next for a temporal ultrasonic study to sort things out, which would then need to be incorporated by The Planner into the user’s life, considering the user’s insurance status, physician networks, schedule, etc., all explained to the user by The Guide.
Example: Hematocrit Result Leads to Sleep Apnea Treatment
To show these agents in action, here’s how a real-world scenario might work, with the four agents collaborating to get to the bottom of an abnormal lab value.
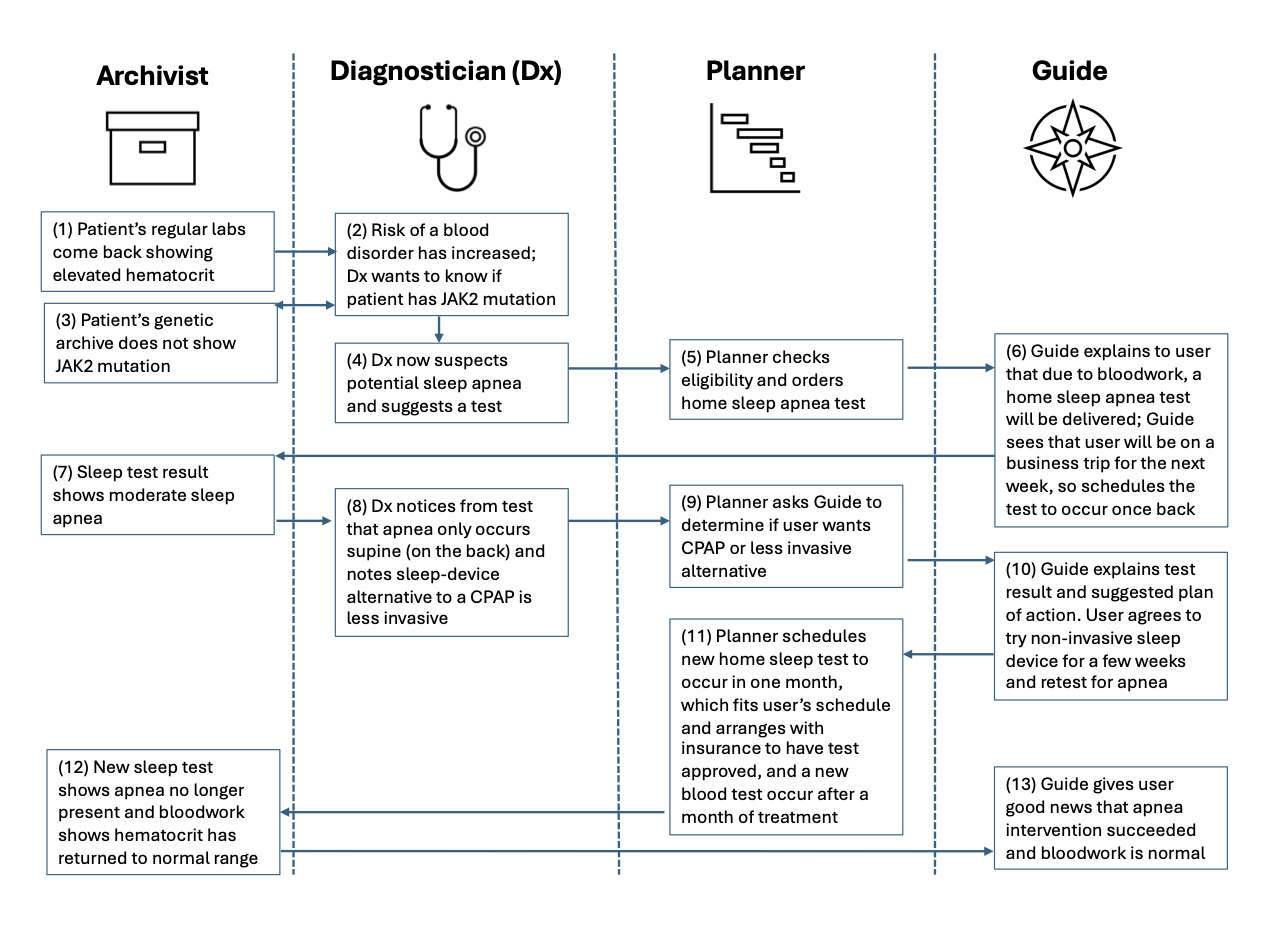
This hypothetical example may or may not relate to how the author of this post spent the last two months figuring out a similar issue (thanks to the care team at Firefly). An agentic future would make this sequence even more seamless, ensuring that the archive, the risk assessment, the health plan, and the user’s mindset are cared for at every step of the journey, possibly without the need for human intervention. Importantly, an AI-driven model would remove much – if not all – of the human costs, liberating the model from process bottlenecks and resource constraints.
Innovation as the Path to this Future
This sci-fi vision of the future may be closer than one might think. Companies like Zus and Health Gorilla already handle much of the tasks of an Archivist, as does Apple Health to a large degree for consumers (for entities that are properly linked). The Diagnostician already exists in the form of Google’s MedPalm models, and its AI rivals are not far behind. One already can upload an archive to these models to seek medical analysis. The Planner has further to go, but the venture market is replete with pitch decks of companies aiming to deploy agents to take over every administrative task in healthcare from answering the phone (e.g., Clarion or Hyro), to preauthorizing care (e.g. Cohere), to handling the billing (e.g. Akasa).
If doctors can have a bots call patients to remind them of appointments, why can’t patients have bots take the call and schedule care for when its suits their busy lives (in sync with health plan requirements)? As for The Guide, this may be the most Black Mirror-esque component, but most people would benefit from an always-on agent like Scarlett Johansson in Her, who simply takes care of everything. The ChatGPT voice is along those lines; just imagine the power of that interface when linked to the other three agents, entities who can actually “figure it out” and “get it done.” It’s not too hard to imagine Apple rolling out an “Apple Health+”* service that leverages AI and the iPhone’s health archive to assess risks and help users get care; other wearables such as Oura Ring may also go down a similar path.
Linking Back to our Terrestrial System of Care
How this AI future will integrate with our existing “terrestrial health system” remains an open question. And by “terrestrial,” I’m referring to all the buildings, offices, devices, labs, imaging centers, insurance companies, pharmacies, and HR departments that make up more than 18% of U.S. GDP. Those organizations already have a head start adopting AI tools to make their work more efficient, effective, and scalable, aided by countless health tech startups and established companies. As noted in a prior post on The New Digital Care Architecture, in order for data to take a full seat at the table alongside doctors, drugs, and diagnostics, a myriad of technologies and processes need to evolve, including advances in both AI and the interoperability enabled by APIs.
These Four Agents represent something more personal – a model by which each person can have guardian angels in the cloud, always thinking about their health, meeting them where they are, to get them the care they require; anticipating what they need next often before they realize it. The implications for how personalized agents would extend from, interact with, and refine our existing health system remain unclear and are an area ripe for innovation. Though much of the “how” in this vision is unclear, what is clear is that the advance of AI agents will make much of care radically cheaper, more accessible, and more convenient.
So What?
In the coming months, more of the “so what” will be explored, aiming to identify actionable projects that can bring about this much more active, effective, scalable, and affordable healthcare future. If we can create real markets for care, where providers and individuals manage budgets to optimize health in tune with the personal needs of users, creative destruction will be unleashed to reshape our system for the better.
Of course, manifold risks must be managed and dealt with as we build a new healthcare future, rooted in AI systems such as these. That’s why we need entrepreneurs, clinicians, regulators, and operators to collaborate in the pursuit of “doing well by doing good.” for the sake of us all. If venture investors can help pull this future forward faster by financing the work, all the better.